Hypertrophic Dermal Reaction:
Hypertrophic Dermal Reaction
For many decades, a wrong terminology has been used to define a process that occurs after injury, often surgical injury to the skin, whereby the site of injury or the surgical incision becomes minimally swollen, i.e. hypertrophic. This reaction, - which at times resolves on its own, or transforms into a keloid - has been erroneously called “hypertrophic scarring”.
The correct terminology for this abnormal wound healing reaction is Hypertrophic Dermal Reaction. The term “scar” defines a permanent mark on the skin after a wound has fully healed. Acne scarring is a good example of marks left on the skin from acne. Acne scarring is not used to define a newly formed acne lesion on the face. Same logic applies to Hypertrophic Dermal Reaction that occurs within the first few weeks or months after wounding of the skin. The appearance of this reaction is a visibly raised inflammatory tissue that forms along the surgical incision lines.
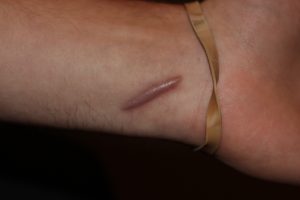
Hypertrophic Dermal Reaction is most likely due to the same genetic disorder that keloid patients have, but in a very mild form. The image below depicts a case of Hypertrophic Dermal Reaction.
Keloid disorder is a complex genetic illness that predisposes individuals to form keloid lesions. Although we still do not know the exact genetic abnormality(ies) that cause this illness, we fully understand that this genetic predisposition has a wide spectrum. As a result, there are individuals who suffer from mild form of the disorder who in their lifetime only develop Hypertrophic Dermal Reaction, or one or few slow-growing keloidal lesions. Also, there are patients who develop very severe form of the disorder and end up with numerous large keloids. There are also many individuals who fall somewhere in between the two extremes.
Most Hypertrophic Dermal Reactions improve over time, even without any treatment. Steroid injections can expedite the healing process and reduce the swelling of these reactions. Below is a video recording of intralesional steroid injections and treatment of a 2 weeks old skin wound in a patient who had developed a mild form of hypertrophic dermal reaction.
This patient was known to have keloid disorder. The dermal reaction to the injury within two weeks already looked like it was transforming into a keloid. In this case, Dr. Tirgan injected the length of the wound with very low dose steroid, in order to prevent keloid formation. At a follow-up visit a few weeks later, the skin appeared completely flat and without any evidence of keloid formation.